If abused, oxycodone can cause serious problems, including overdose, coma, breathing issues, and even death.
It is an addictive prescription medication that should not be underestimated.
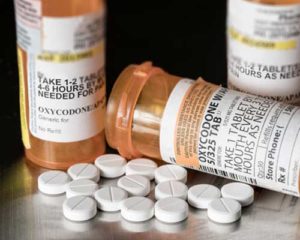
Oxycodone Overview
Oxycodone is an opioid painkiller, only available via prescription.
Oxycodone comes in a variety of forms, such as Endocet and OxyContin, which may mix oxycodone with another drug like acetaminophen. When taking medications like these, it is essential to use them correctly because of oxycodone’s opioid properties.
Oxycodone abuse is a danger with any oxycodone prescription. As an opioid, oxycodone is highly addictive and prone to misuse. Patients with a history of drug abuse, especially opioid abuse, should not be administered oxycodone unless deemed necessary.
When a patient is abusing oxycodone, they are taking it not in prescribed dosages. There are a few guidelines that signal abuse, and this is one of them. According to the Mayo Clinic, an adult prescribed oxycodone will usually begin on a dose of 9 mg every 12 hours, which a doctor may eventually rise to as much as 288 mg per day. The dosages for children and those tolerant to opioids will vary more widely.
Oxycodone is a potent drug. Only take it as prescribed.
Why Do People Abuse Oxycodone?
Oxycodone is designed to block pain by triggering endorphins. Endorphins make a person feel a sense of euphoria, and they dull pain. The same property that makes oxycodone good at fighting pain makes it prone to abuse.
When abused, oxycodone can be used to trigger a chemically induced sense of extreme euphoria and pain relief. This endorphin-release process gets very addictive. The brain craves that sense of well-being when the high from the oxycodone or similar drugs begins to fade.
Thus, a cycle of abuse easily develops. Oxycodone makes the user feel good, and they grow addicted to that feeling. They also have to contend with the fact that they legitimately feel worse once the effect fades.
This becomes a serious issue as the abuse continues. The person grows more tolerant and needs increasing amounts of oxycodone to chase that same feeling of euphoria.
What pushes people to abuse oxycodone varies widely. Often, it can begin with a legitimate prescription for pain from a doctor that then spirals out of control.
If you are prescribed oxycodone, be very careful with your prescription. Talk with your doctor if you feel your prescribed dose is no longer effective. Do not attempt to increase the dose or frequency with which you take the medication on your own.
Oxycodone Overdose
The Substance Abuse and Mental Health Services Administration (SAMHSA) has laid out a helpful guide to help people who take opioids (as prescribed or otherwise), and their families prevent overdose.
SAMHSA notes two important categories of symptoms in which to watch out. The first are signs of overmedication, meaning that a person is (willfully or accidentally) taking more medication than they should be. This type of use can easily lead to an overdose.
Signs of overmedication include:
- Confusion or strange speech patterns
- Unusual drowsiness
- Slowed breathing
- Eye miosis (tiny pupils)
- Slowed heartbeat or low blood pressure
- Difficulty to awaken
These symptoms are serious and should be brought up to a doctor as soon as possible. Many are precursors to dangerous and even lethal overdose symptoms.
Regardless of whether overmedication signs were initially noticed or not, if someone on oxycodone shows the following signs, they are likely overdosing:
- The person cannot speak or seems extremely disoriented
- They have bluish or purplish lips or fingernails
- They are limp or comatose
- They are gurgling or vomiting
- Their heart has dangerously slowed or stopped beating altogether
- The person is not breathing, or their breathing is extremely shallow
Call 911 immediately if you observe any of these symptoms of overdose.
What To Do
In the case of an oxycodone overdose or even a suspected overdose, begin the following steps immediately:
- Call 911 and report your location, the nature of the overdose, and any known medical details about the person who is overdosing.
- If available, administer naloxone (discussed below) as soon as possible. If the person overdosing is conscious, ask if they know if naloxone is available.
- Administer emergency aid as necessary while trying to answer any questions the 911 operator asks.
- Administer emergency breathing if the person is not breathing but still has a heartbeat.
- Administer CPR if the person’s heart has stopped. If another person is available, take turns with chest compressions to avoid fatigue.
Naloxone
If you are taking any opioid, oxycodone included, discuss naloxone with your doctor. If you receive it, keep it in a safe place you can access whenever you are taking opioids.
Naloxone is an opioid antagonist.
This means it reverses the dangerous effects of opioids. Although it can have some uncomfortable side effects, such as sweating and hot flashes, its ability to potentially reverse an opioid overdose saves lives.
Naloxone doesn’t last as long in the body as other opioids. If it wears off before the opioids of abuse do, the overdose can return. As a result, further medical attention is needed after naloxone is administered.
Opioid overdoses can be severe. It is likely that you will be unable to administer naloxone yourself if you are experiencing an overdose.
Keep your family and those in your home informed of its location and how to administer it if necessary.
Get Help
Naloxone is not a pass to abuse opioids. Oxycodone can be deadly. Overdose can cause long-term damage, especially if the brain doesn’t get enough oxygen for a significant amount of time.
If you have problems abusing opioids, seek help. Naloxone can be a useful tool in emergencies but overcoming your addiction will dramatically improve your life. Treatment could save you from a future life-threatening overdose.
